12) Baseline left ventricular ejection fraction was determined using two-dimensional echocardiography performed before or after PCI. The estimated glomerular filtration rate was calculated using the Modification of Diet in Renal Disease study equation. All laboratory findings were performed upon admission, except for lipid profiles, which were obtained after at least 9 hours of fasting within 24 hours of hospitalization.

The diagnosis of ST-segment elevation myocardial infarction (STEMI) was based on ST-segment elevation>2 mm in at least two precordial leads, ST-segment elevation>1 mm in at least two limb leads, or new left bundle branch block on a 12-lead electrocardiogram in the infarct-related artery distribution, as determined by coronary angiography with increased cardiac-specific biomarkers. A history of renal insufficiency included a history of chronic kidney disease and patients receiving chronic dialysis. The patients' demographics, vital signs on admission, and medical history were compared among groups.

The ethics committee of each participating hospital approved the study protocol, and all patients provided written informed consent.
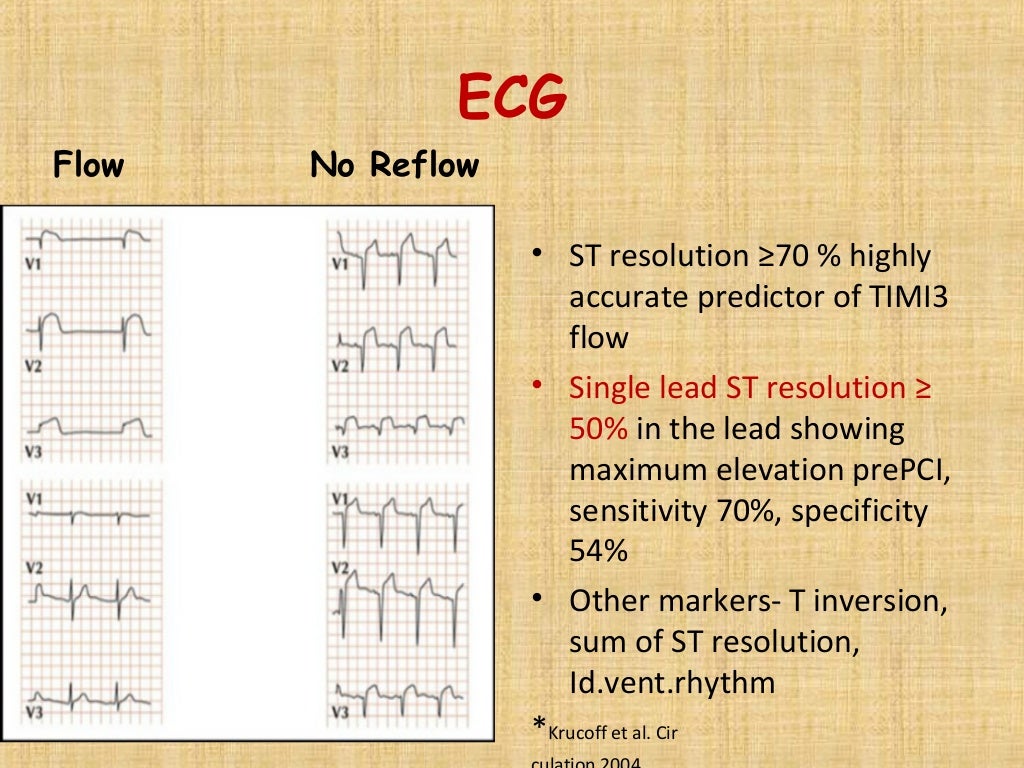
Patients with vasospasm, distal embolism or coronary dissection were excluded. An operator at each center confirmed no reflow during PCI. The no reflow phenomenon was defined as the disruption of coronary flow distal to a treatment segment following initial procedure despite patency of the epicardial coronary arteries after PCI. The remaining subjects were divided into three groups according to the presence of no reflow and post-procedural TIMI flow grade: the normal reflow group was defined as patients without any no reflow who achieved final TIMI flow grade 3 (n=4071) the transient no reflow group was defined as patients having no reflow during PCI who achieved final TIMI flow grade 3 after adequate management of the no reflow (n=213, 4.9% of all patients) and the persistent no reflow group was defined as patients having no reflow whose final TIMI flow grade was ≤2 despite of management for no reflow (n=45, 1.0% of all patients). We excluded 419 patients, including 184, 17, and 97 patients without any no reflow who achieved post-procedural thrombolysis in myocardial infarction (TIMI) flow grades 0, 1, or 2, respectively, 28 patients who did not have coronary stents implanted, and 93 patients with insufficient data. Of the 4748 patients in the COREA-AMI registry, 4329 who underwent PCI with coronary stents were analyzed. The Convergent Registry of Catholic and Chonnam University for AMI (COREA-AMI) is a Korean prospective, multicenter, observational registry that was designed to reflect real-world practice in Korean AMI patients at nine centers with facilities for primary PCI, representing two universities, between January 2004 and December 2009. Therefore, this study investigated the incidence of transient or persistent no reflow during PCI, its clinical and angiographic characteristics, and the long-term clinical outcomes in patients with AMI based on a Korean multicenter registry. 8), 9), 10), 11) Furthermore, no studies have examined the long-term clinical outcomes according to the persistence of no reflow.
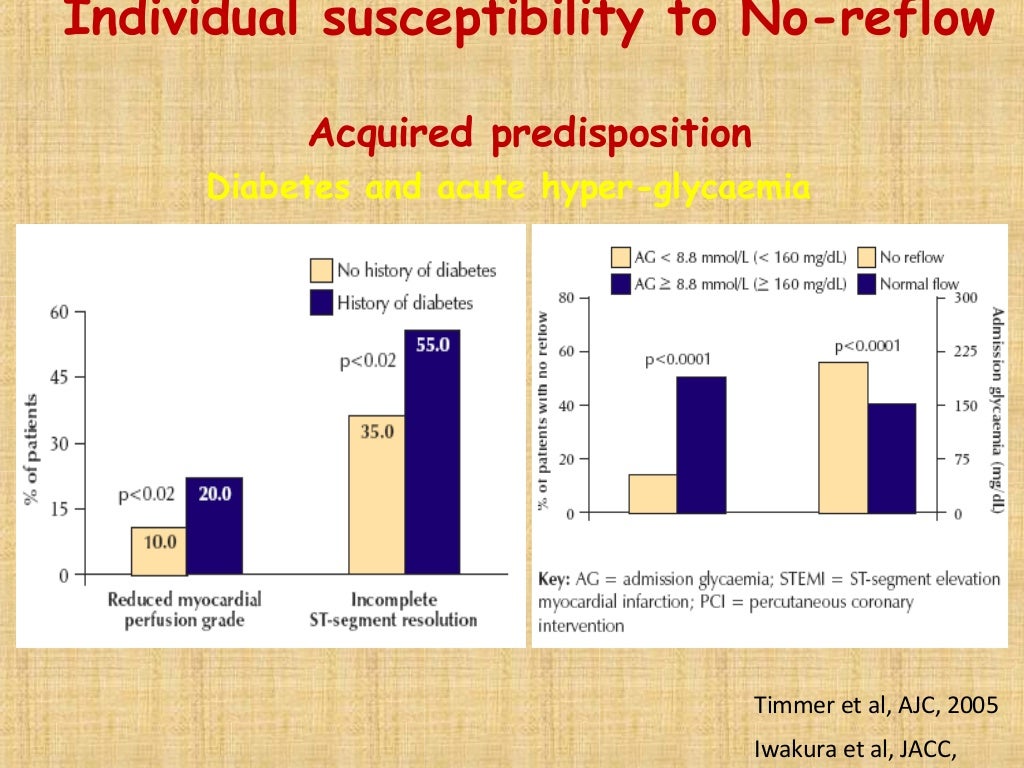
However, few studies have described the incidence and prognosis of transient or persistent no reflows in patients with AMI. 1) Although interventional cardiologists try to overcome no reflow using various methods and drugs, 2) persistent no reflow often remains despite adequate revascularization of coronary stenosis. The pathomechanism of no reflow includes ischemia-reperfusion injury, myocardial edema, endothelial swelling, capillary obstruction, vasospasm, inflammatory response, and distal coronary embolization. 1), 2) No reflow negatively affects the clinical outcome in patients with acute myocardial infarction (AMI), 3), 4), 5), 6) and it is associated mainly with increased mortality or left ventricular remodeling, despite its relatively low incidence. It is defined as a state of myocardial hypoperfusion in the presence of a patent epicardial coronary artery. The no reflow phenomenon is a serious complication following percutaneous coronary intervention (PCI).
